September 2021
Heel Pain
Heel pain can be difficult to deal with, especially if you do not know what the underlying cause is. If you ignore your heel pain, the pain can magnify and potentially develop into a chronic condition. Depending on the location of your heel pain, you have developed a specific condition.
One condition is plantar fasciitis. Plantar fasciitis is caused by the inflammation of the plantar fascia, or the band of tissue that connects the heel bone to the base of the toes. The pain from this condition is initially mild but can intensify as more steps are taken when you wake up in the morning. To treat this condition, medication will likely be necessary. Plantar fasciitis is often associated with heel spurs; both require rest and special stretching exercises.
There are various options your podiatrist may suggest for heel pain. Treatment options for heel pain typically include non-steroidal anti-inflammatory drugs (NSAIDS), which may reduce swelling and pain. Other options are physical therapy, athletic taping, and orthotics. In severe cases of heel pain, surgery may be required.
Preventing heel pain is possible. If you are looking to prevent heel pain from developing in the future, be sure to wear shoes that fit you properly and do not have worn down heels or soles. Be sure to warm up properly before participating in strenuous activities or sports that place a lot of a stress on the heels. If you are experiencing any form of heel pain, speak with your podiatrist to determine the underlying cause and receive the treatment you need.
Should I See a Doctor for My Heel Pain?
 Heel pain is one of the most common conditions podiatrists help treat, and it can have a variety of causes. Common causes of heel pain include plantar fasciitis, Achilles tendonitis, bursitis, a ruptured Achilles tendon, or a heel fracture. There are a few key signs that your heel pain may be serious and needs to be checked by a podiatrist. If the pain continually worsens, stops you from doing daily activities, has not improved after a couple of weeks, or causes a tingling sensation in the heel, there may be a more serious issue at play that should be checked by a podiatrist. If the pain is severe, hinders your ability to walk, or was accompanied by a popping sensation at the time of injury, these may be signs of an even more serious injury that should be treated immediately.
Heel pain is one of the most common conditions podiatrists help treat, and it can have a variety of causes. Common causes of heel pain include plantar fasciitis, Achilles tendonitis, bursitis, a ruptured Achilles tendon, or a heel fracture. There are a few key signs that your heel pain may be serious and needs to be checked by a podiatrist. If the pain continually worsens, stops you from doing daily activities, has not improved after a couple of weeks, or causes a tingling sensation in the heel, there may be a more serious issue at play that should be checked by a podiatrist. If the pain is severe, hinders your ability to walk, or was accompanied by a popping sensation at the time of injury, these may be signs of an even more serious injury that should be treated immediately.
Many people suffer from bouts of heel pain. For more information, contact Corinne R. Kauderer, DPM of Dyker Heights Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact one of our offices located in Brooklyn, NY and Old Bridge, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds, and every 19 minutes, an older person dies from falling. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
The Consequences of a Fall
Falls are the leading cause of injury and hospitalizations in older adults across North America. Most falls occur in the home, due to slipping or stumbling. Falls can result in both minor and major injuries, from bruises and sprains to dislocations and fractures. Injuries sustained from a fall can make falling in the future more likely, as they can impair mobility and decrease an older adult’s self-confidence when it comes to getting around their home and community. There are several steps that you can take to prevent falls, including removing tripping hazards from the home, installing non-slip mats and grab bars in slippery areas, and using a mobility aid when needed. To learn more about preventing falls, please consult with a podiatrist.
Preventing falls among the elderly is very important. If you are older and have fallen or fear that you are prone to falling, consult with Corinne R. Kauderer, DPM from Dyker Heights Foot & Ankle. Our doctor will assess your condition and provide you with quality advice and care.
Every 11 seconds, an elderly American is being treated in an emergency room for a fall related injury. Falls are the leading cause of head and hip injuries for those 65 and older. Due to decreases in strength, balance, senses, and lack of awareness, elderly persons are very susceptible to falling. Thankfully, there are a number of things older persons can do to prevent falls.
How to Prevent Falls
Some effective methods that older persons can do to prevent falls include:
- Enrolling in strength and balance exercise program to increase balance and strength
- Periodically having your sight and hearing checked
- Discuss any medications you have with a doctor to see if it increases the risk of falling
- Clearing the house of falling hazards and installing devices like grab bars and railings
- Utilizing a walker or cane
- Wearing shoes that provide good support and cushioning
- Talking to family members about falling and increasing awareness
Falling can be a traumatic and embarrassing experience for elderly persons; this can make them less willing to leave the house, and less willing to talk to someone about their fears of falling. Doing such things, however, will increase the likelihood of tripping or losing one’s balance. Knowing the causes of falling and how to prevent them is the best way to mitigate the risk of serious injury.
If you have any questions, please feel free to contact one of our offices located in Brooklyn, NY and Old Bridge, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is an enlargement of the base joint of the toe that connects to the foot, often formed from a bony growth or a patch of swollen tissues. It is caused by the inward shifting of the bones in the big toe, toward the other toes of the foot. This shift can cause a serious amount of pain and discomfort. The area around the big toe can become inflamed, red, and painful.
Bunions are most commonly formed in people who are already genetically predisposed to them or other kinds of bone displacements. Existing bunions can be worsened by wearing improperly fitting shoes. Trying to cram your feet into high heels or running or walking in a way that causes too much stress on the feet can exacerbate bunion development. High heels not only push the big toe inward, but shift one's body weight and center of gravity towards the edge of the feet and toes, expediting bone displacement.
A podiatrist knowledgeable in foot structure and biomechanics will be able to quickly diagnose bunions. Bunions must be distinguished from gout or arthritic conditions, so blood tests may be necessary. The podiatrist may order a radiological exam to provide an image of the bone structure. If the x-ray demonstrates an enlargement of the joint near the base of the toe and a shifting toward the smaller toes, this is indicative of a bunion.
Wearing wider shoes can reduce pressure on the bunion and minimize pain, and high heeled shoes should be eliminated for a period of time. This may be enough to eliminate the pain associated with bunions; however, if pain persists, anti-inflammatory drugs may be prescribed. Severe pain may require an injection of steroids near the bunion. Orthotics for shoes may be prescribed which, by altering the pressure on the foot, can be helpful in reducing pain. These do not correct the problem; but by eliminating the pain, they can provide relief.
For cases that do not respond to these methods of treatment, surgery can be done to reposition the toe. A surgeon may do this by taking out a section of bone or by rearranging the ligaments and tendons in the toe to help keep it properly aligned. It may be necessary even after surgery to wear more comfortable shoes that avoid placing pressure on the toe, as the big toe may move back to its former orientation toward the smaller toes.
Are Bunions Noticeable?
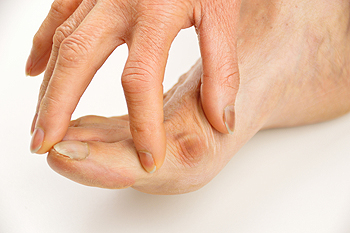 It is generally easy to notice a bunion when it has developed on your foot. A bunion is a bump that forms on the side of the big toe that can make wearing shoes difficult for the majority of the day. A common reason why bunions can form is from wearing shoes that do not have adequate room for the toes to move freely in. Additionally, they may form from genetic reasons. If the bunion grows, it can change the shape of the foot, and larger shoes may need to be purchased. Ballet dancers are often at risk of developing bunions because of the constant stress the feet endure while practicing specific poses. Pregnancy can lead to the formation of bunions, which may come from hormonal changes that can affect the feet. Mild relief may be found when a protective pad is worn over the bunion, and this can be helpful in protecting it against friction that can come from wearing shoes. If you notice a bump has formed on your foot, it is strongly suggested that you consult with a podiatrist who can perform a proper diagnosis and offer you correct treatment methods.
It is generally easy to notice a bunion when it has developed on your foot. A bunion is a bump that forms on the side of the big toe that can make wearing shoes difficult for the majority of the day. A common reason why bunions can form is from wearing shoes that do not have adequate room for the toes to move freely in. Additionally, they may form from genetic reasons. If the bunion grows, it can change the shape of the foot, and larger shoes may need to be purchased. Ballet dancers are often at risk of developing bunions because of the constant stress the feet endure while practicing specific poses. Pregnancy can lead to the formation of bunions, which may come from hormonal changes that can affect the feet. Mild relief may be found when a protective pad is worn over the bunion, and this can be helpful in protecting it against friction that can come from wearing shoes. If you notice a bump has formed on your foot, it is strongly suggested that you consult with a podiatrist who can perform a proper diagnosis and offer you correct treatment methods.
If you are suffering from bunion pain, contact Corinne R. Kauderer, DPM of Dyker Heights Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact one of our offices located in Brooklyn, NY and Old Bridge, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Are Bunions Affecting Your Everyday Life?
Arthritic Foot Care
During your lifetime, you will probably walk about 75,000 miles, which is quite a lot of stress to put on your feet. As you get older, the 26 bones and 30 joints in each of your feet will lose flexibility and elasticity. Your foot’s natural shock absorbers will wear down as well. Having arthritis added to this mix only makes matters worse. Your joints will become distorted and inflamed, which is why arthritic foot care needs to be something to think about every day.
When dealing with arthritis, having additional foot complications, such as bunions, hammertoes, or neuroma, can be a serious detriment. To avoid these, buy well-fitting shoes with a lower heel and good support. Arthritis causes you to lose your arch, so having shoes with good arch support is also highly recommended.
Aside from getting good arch support, the shoes need to fit comfortably and properly as well. A good place to start is by leaving a finger width between the back of the shoe and your foot to gauge proper size. It is also helpful to have a square or rounded toe box in the front to provide even more comfort. Another thing to look for is a rubber sole that can provide a cushion and absorb shock as you walk. This adds flexibility to the ball of your foot when you push off your heel to walk.
Exercise is another key aspect of arthritic foot care. Exercise not only strengthens and stretches your muscles and joints, but helps to prevent further injury and pain as well. Stretching the Achilles tendon, the tendon located in the back of your heel, will give you added mobility and reduce pain due to stress. Another thing you can do is massage your feet, kneading the ball of your foot as well as your toes from top to bottom.
Stretching the Achilles tendon is a simple exercise that you can do at home anytime. Lean against the wall with your palms flat against the surface while placing one foot forward, towards the wall, and one foot behind you. Bend your forward knee towards the wall while keeping your back knee locked straight, and make sure both your heels are completely touching the ground at all times. This will stretch your Achilles tendon and calf muscles as well. You will feel the stretch almost immediately. You can also stretch your toes in a couple ways. One involves taking a rubber band and wrapping it around both your big toes while your heels remain together. Then, pull them apart to stretch your big toe. You can also place a rubber band around all the toes of one of your feet. Then, try to separate each individual toe, stretching them all.
A final step you can take to help your arthritis is taking non-steroid, non-inflammatory drugs or topical medicines with capsaicin. Unfortunately, there is no complete way to remove all of your arthritic pain. However, following some of this advice can go a long way in staying as pain-free as possible.
Psoriatic Arthritis and the Feet
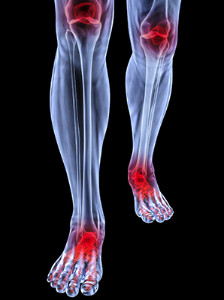 Psoriatic arthritis is a type of arthritis that affects people who have a skin condition called psoriasis. Like other types of arthritis, psoriatic arthritis is characterized by joint pain, stiffness, and swelling. It can affect nearly any joint in the body, but often affects the joints of the feet and ankles. In addition to joint pain, symptoms of psoriatic arthritis in the feet can include pain in the heel and arch of the foot due to enthesitis, an inflammation of the points where tendons and ligaments attach to bones. People with this type of arthritis are also more likely to have nail problems, such as nail pitting and thickening, pain, and lifting of the nail from the nailbed. If you have psoriatic arthritis that affects your feet, a podiatrist can help by prescribing treatments and orthotics that can reduce symptoms and improve mobility. To learn more, please consult with a podiatrist.
Psoriatic arthritis is a type of arthritis that affects people who have a skin condition called psoriasis. Like other types of arthritis, psoriatic arthritis is characterized by joint pain, stiffness, and swelling. It can affect nearly any joint in the body, but often affects the joints of the feet and ankles. In addition to joint pain, symptoms of psoriatic arthritis in the feet can include pain in the heel and arch of the foot due to enthesitis, an inflammation of the points where tendons and ligaments attach to bones. People with this type of arthritis are also more likely to have nail problems, such as nail pitting and thickening, pain, and lifting of the nail from the nailbed. If you have psoriatic arthritis that affects your feet, a podiatrist can help by prescribing treatments and orthotics that can reduce symptoms and improve mobility. To learn more, please consult with a podiatrist.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Corinne R. Kauderer, DPM from Dyker Heights Foot & Ankle. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions, please feel free to contact one of our offices located in Brooklyn, NY and Old Bridge, NJ . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.